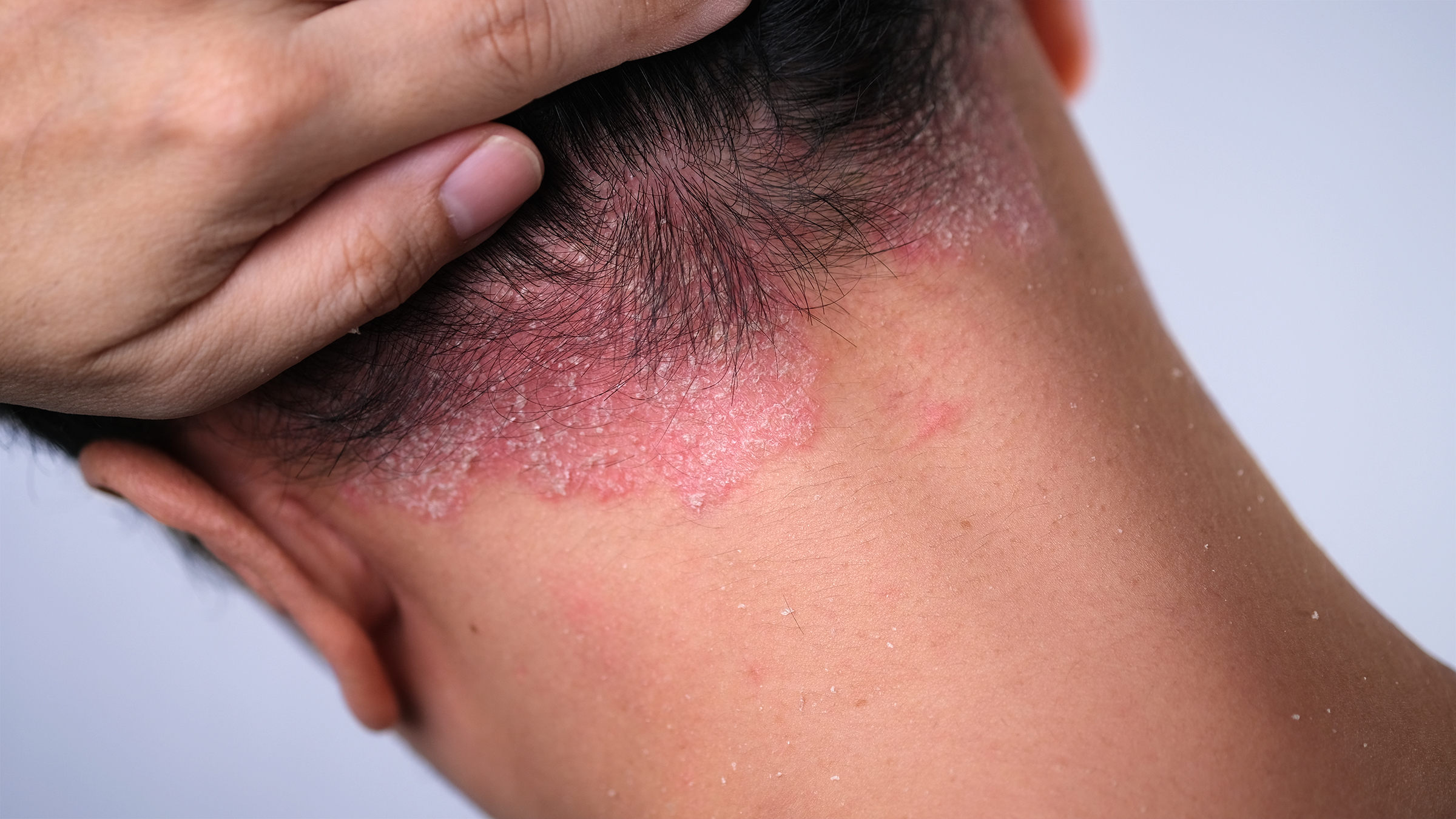
What is plaque psoriasis?
Plaque psoriasis is the most common form of psoriasis, accounting for approximately 80-90% of all psoriasis cases. It is characterized by rapid growth of skin cells, resulting in thick, silvery-white, scaly patches or plaques on the surface of the skin. These patches typically appear on the elbows, knees, scalp, and lower back, and can develop anywhere in the body.
Psoriasis is an autoimmune disease, which means that the immune system mistakenly attacks healthy skin cells. In plaque psoriasis, this immune response speeds up the life cycle of skin cells, causing cells to rapidly accumulate on the surface of the skin. This abnormal growth results in the distinctive plaques associated with the disease.
Symptoms of plaque psoriasis
Symptoms of plaque psoriasis vary widely in severity and may include:
Red patches of skin covered with thick, silvery scales: The hallmark of plaque psoriasis is red, inflamed patches covered with silvery-white scales. These patches or plaques may itch and be painful, and sometimes even crack and bleed.
Dry, cracked skin that may bleed: Excessive buildup of skin cells can cause the skin to become extremely dry and crack easily. When these cracks appear, they may be painful and bleed.
Itching, burning, or soreness: The inflammation and rapid skin cell turnover associated with plaque psoriasis can cause significant discomfort, like itching, burning, and soreness.
Thickened, pitted, or ridged nails: Psoriasis can affect the nails, causing them to become thickened, pitted, or ridged. The nails of seriously ill patients may separate from the nail bed.
Swelling and stiff joints: Psoriasis is associated with psoriatic arthritis, a disease that causes joint swelling and stiffness. This symptom is the systemic nature of the disease.
Small scaly patches (common in children): In some cases, especially in children, plaque psoriasis may present as small, scaly patches rather than large plaques.
Silent but deadly: Systemic effects
While plaque psoriasis has obvious outward symptoms, the effects of this disease extend far beyond the skin. Psoriasis is a systemic disease, and it affects the entire body, not just the skin. This systemic nature makes it a potentially fatal disease, especially if left untreated or poorly managed.
Increased Risk of Cardiovascular Disease:
People with plaque psoriasis are at higher risk for cardiovascular disease, such as heart attack and stroke. Chronic inflammation, a hallmark of psoriasis, is an important factor in this increased risk.
Metabolic Syndrome:
Plaque psoriasis is associated with metabolic syndrome, a group of conditions that include obesity, high blood pressure, high blood sugar, and abnormal cholesterol levels. This syndrome increases the risk of heart disease, diabetes, and stroke.
Mental Health Disorders:
The psychological impact of plaque psoriasis can be profound. Many people with the disease experience depression, anxiety, and social isolation because of the significant nature of the symptoms and the stigma associated with the disease.
Psoriatic Arthritis:
As mentioned previously, a large number of people with plaque psoriasis will develop psoriatic arthritis, a painful and potentially disabling disease that affects the joints. Early diagnosis and treatment are essential to prevent joint damage and improve life quality.
Inflammatory bowel disease:
There is an increasing prevalence of inflammatory bowel diseases such as Crohn's disease and ulcerative colitis among people with plaque psoriasis. This comorbidity highlights the systemic inflammatory nature of the disease.
Early diagnosis and treatment:
Early diagnosis and effective treatment are essential to managing plaque psoriasis and minimizing its following influences. If you suspect you have plaque psoriasis, it is crucial to see a doctor promptly. A dermatologist can diagnose the condition based on a physical exam and, in some cases, a biopsy.
Treatment for plaque psoriasis aims to reduce inflammation, slow the rapid turnover of skin cells, and manage associated symptoms. A treatment plan may include:
Topical treatments: Topical treatments such as corticosteroids, vitamin D analogs, and retinoids are usually the first line of treatment for mild to moderate plaque psoriasis. These medications help reduce inflammation and slow skin cell growth.
Phototherapy: Phototherapy, or phototherapy, involves exposing the skin to ultraviolet (UV) light under medical supervision. This treatment can help reduce symptoms and improve the appearance of the skin.
Systemic medications: For moderate to severe plaque psoriasis, systemic medications that are effective throughout the body may be needed. These include oral or injectable medications such as methotrexate, cyclosporine, and biologics. Biologics are a new kind of medications that target specific parts of the immune system to reduce inflammation.
Lifestyle changes: Lifestyle modifications play an important role in the management of plaque psoriasis. There are several ways to improve symptoms and overall health, such as maintaining a healthy diet, exercising regularly, avoiding smoking, and managing stress.
Support and counseling:
Given the psychological impact of plaque psoriasis, support groups, and counseling may be necessary and beneficial. Communicating with others who have similar experiences and receiving professional mental health support can improve quality of life.
Conclusion
Plaque psoriasis is a chronic autoimmune disease that seriously affects the skin and overall health. Its symptoms, including red, scaly plaques and itching, are often visible and uncomfortable. However, the systemic nature of the disease means that it can have serious effects on cardiovascular health, mental health, and joint function.
Early diagnosis and comprehensive treatment are essential to managing plaque psoriasis and reducing its systemic effects. If you suspect you have plaque psoriasis, seeking medical help and sticking to a treatment plan can help control symptoms and improve quality of life. Additionally, lifestyle changes and mental health support also play a vital role in managing this complex disease.
Understanding plaque psoriasis as a silent but potentially deadly disease underscores the importance of increased awareness, early intervention, and a holistic approach to management. With proper care and support, people with plaque psoriasis can live healthier, more fulfilling lives.