What is urinary incontinence?
Urinary incontinence occurs when the muscles that control the bladder do not function properly, resulting in the accidental leakage of urine. This condition can range from occasional minor leaks to frequent, severe leaks that interfere with daily life.
Types of urinary incontinence
Understanding the type of urinary incontinence is crucial to determining the right treatment:
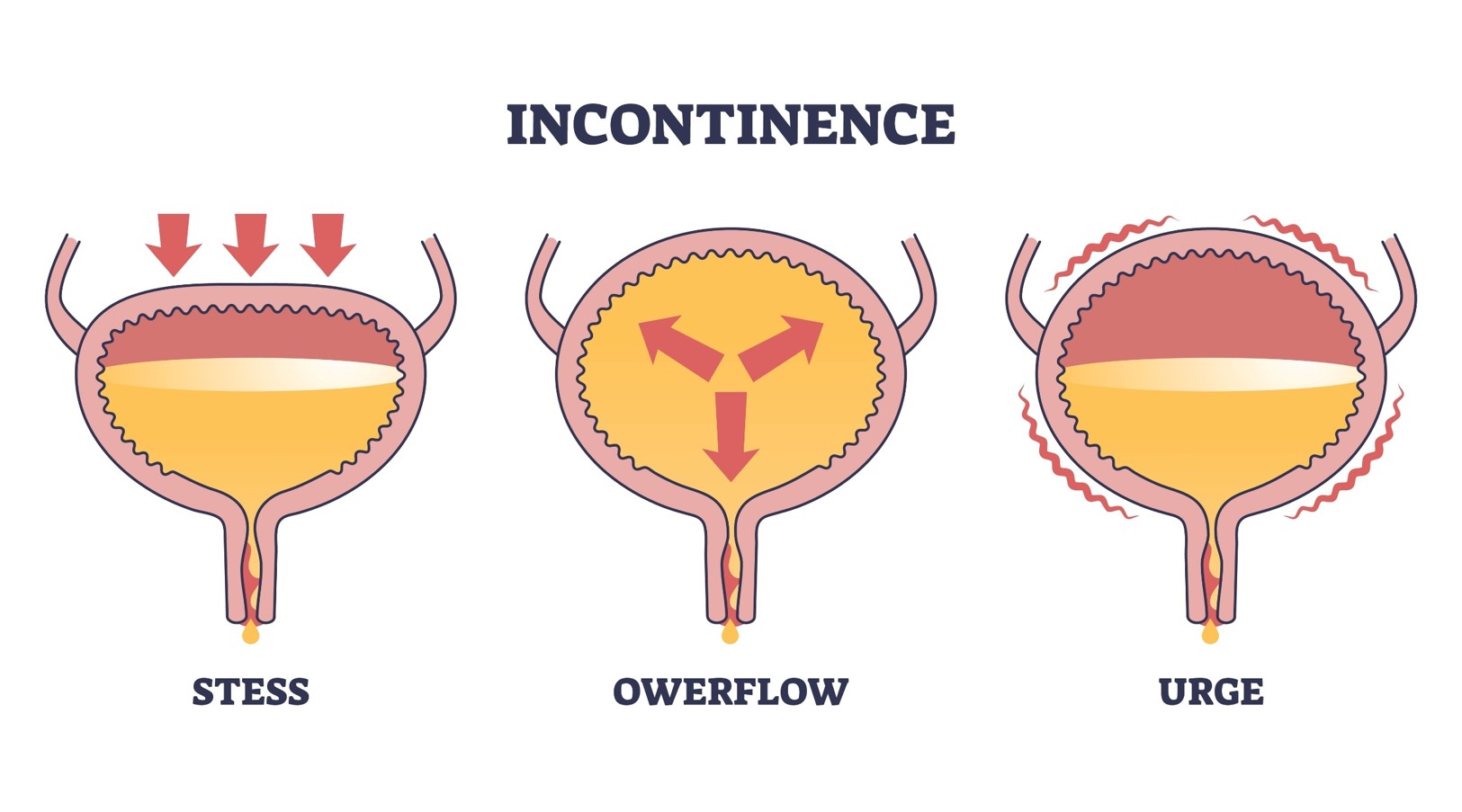
Stress incontinence: Leakage occurs during physical activity such as coughing, sneezing, or exercise that puts pressure on the bladder.
Urge incontinence: A sudden, strong urge to urinate followed by involuntary leakage of urine, often due to an overactive bladder.
Overflow incontinence: The bladder does not empty completely, resulting in frequent or constant dripping of urine.
Mixed incontinence: A combination of symptoms of stress and urge incontinence.
Functional incontinence: A physical or cognitive condition (such as arthritis or dementia) that prevents you from getting to the bathroom in a timely manner.
Common causes of urinary incontinence
Incontinence can be caused by a variety of factors, including:
Aging: Loss of strength in the bladder and pelvic floor muscles.
Pregnancy and childbirth: Hormonal changes and pelvic muscle strain.
Menopause: Declining estrogen levels can weaken bladder control.
Chronic conditions: Diabetes, obesity, and neurological disorders.
Medications: Certain medications can affect bladder function.
Urinary tract infection (UTI): An infection can temporarily disrupt bladder control.
Early warning signs of incontinence
Identifying incontinence early can help you seek medical intervention promptly. Common symptoms include:
Frequent or sudden urges to urinate.
Having trouble getting to the bathroom in time.
Leaking during physical activity or coughing.
A feeling that your bladder is not completely empty.
Treatment options for urinary incontinence
Treatment for urinary incontinence depends on its type and severity. The following are the most common treatments:
1. Change your lifestyle
Bladder training: Delaying urination to increase bladder capacity over time.
Dietary modifications: Avoid caffeine, alcohol, and spicy foods that can irritate the bladder.
Weight management: Lose weight to reduce bladder pressure.
2. Pelvic floor exercises
Also called Kegel exercises, these exercises strengthen your pelvic muscles and improve bladder control. Continued practice can significantly reduce urine leakage.
3. Medication
Anticholinergic drugs: Reduce symptoms of overactive bladder.
Beta-3 adrenergic agonists: Relax the bladder muscles, improving urine storage.
Topical estrogen: Helps restore vaginal and urethral tissue in postmenopausal women.
4. Medical devices
Pessary: A ring-shaped device inserted into the vagina to support the bladder.
Urethral Insert: A temporary plug used to prevent urine leakage during activity.
5. Surgical Intervention
Sling procedure: A mesh sling supports the urethra and helps control leakage.
Bladder neck suspension: A surgical procedure to improve urethral support.
Artificial urinary sphincter: A device implanted in severe cases to control urine flow.
6. Behavioral therapy
Biofeedback: Using sensory feedback to teach bladder muscle control.
Electrical stimulation: Strengthens the pelvic muscles through low-level electrical pulses.
Tips for preventing urinary incontinence
While not all cases can be prevented, practicing healthy habits can reduce your risk:
Perform pelvic floor exercises regularly.
Maintain a healthy weight to minimize stress on your bladder.
Stay hydrated, but avoid overhydration.
Treat urinary tract infections and other conditions promptly.
Avoid smoking, which can cause a chronic cough and a weak bladder.
Conclusion: Take Control of Your Bladder Health
Urinary incontinence is a difficult condition, but with the right approach, it can be controlled and even overcome. From lifestyle adjustments to advanced medical treatments, there are a variety of options to meet individual needs. If you experience symptoms of urinary incontinence, seek medical advice immediately. Early intervention can improve outcomes and significantly enhance your quality of life.
Arm yourself with knowledge and take the first step toward better bladder health today. artificial intelligence